04:05

Down in Starrett City — a neighborhood with a majority of Black and brown residents in Brooklyn, New York — people are mourning for hundreds of lives lost to COVID-19.
With a soaring infection rate and the highest death rate in New York, Starrett evokes a thorny question: if the coronavirus does not discriminate based on race, why are minorities disproportionately dying?
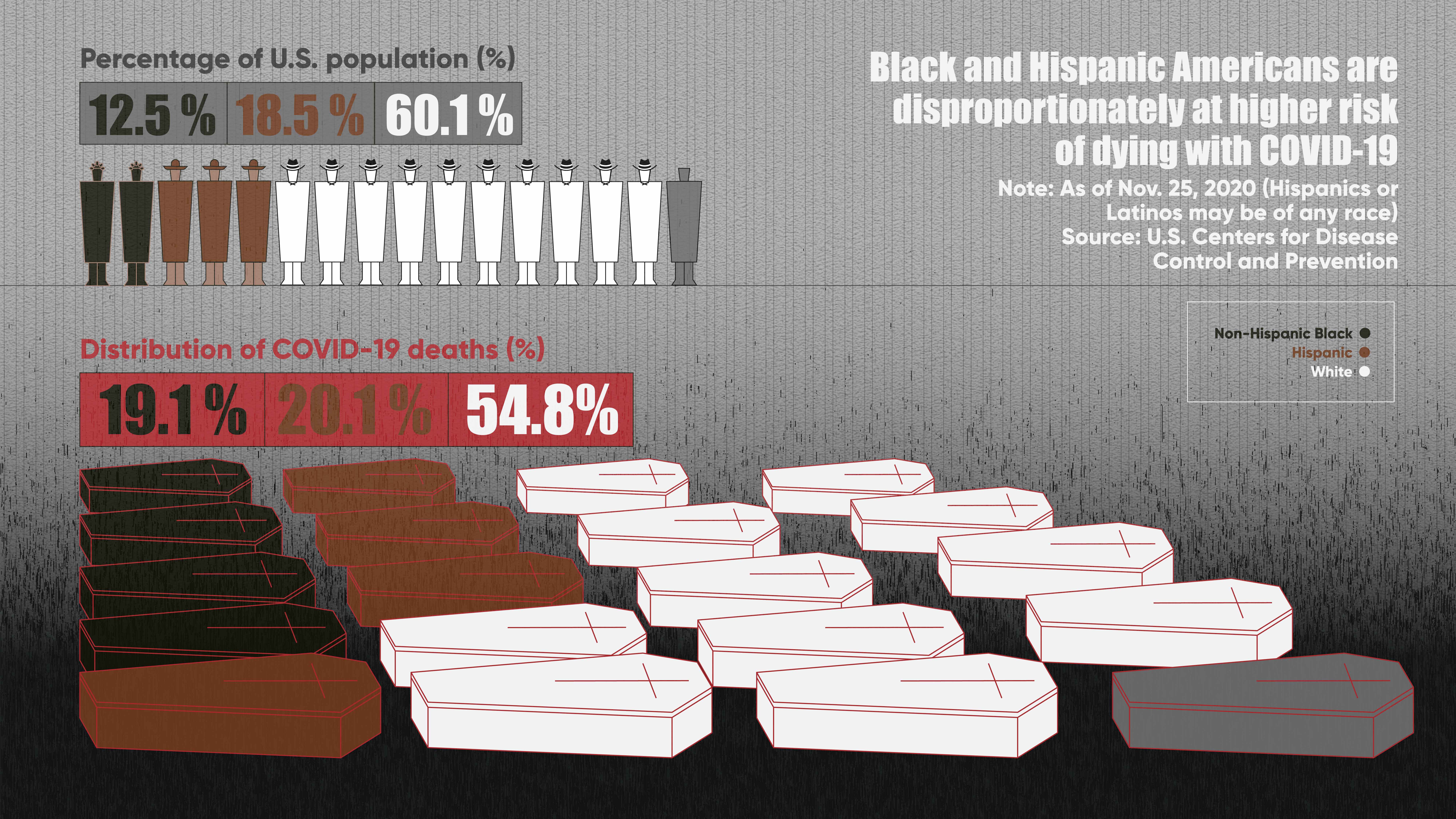
According to the latest U.S. Centers for Disease Control and Prevention report, the non-Hispanic Black community makes up 12.5 percent of the population and 19.1 percent of COVID-19 deaths. And the death rate in the Hispanic community, who make up 18.5 percent of Americans, is 20.1 percent.
So, why are some minority groups in the U.S. more likely to contract COVID-19 and die from it? Is it because they are not wearing masks or don't follow social distancing? Or is it because they are more likely to be obligated to go to work because remote employment is not an option?
U.S. Bureau of Labor statistics suggest Black people are more likely to hold jobs in the medical sector and service industries, which have greater exposure to COVID-19 and can't be done online.
People serving in healthcare settings are more likely to have contact with confirmed COVID-19 patients. Data shows that 37.2 percent of nursing, psychiatric and home health aides are Black. In times when hospitals are under-resourced and understaffed, many of them still jeopardize their lives to fight against COVID-19.
In addition, 35.8 percent of postal service clerks are Black. Like other frontline workers, they cannot work from home. Especially in this election year, more than 90 million people chose to vote by mail, putting postal workers at a high risk of virus exposure. Besides, Black people account for 29.5 percent of taxi drivers and chauffeurs. As long as the taxi companies are still operating, drivers, seating in a confined space with unknown passengers, are on the edge of contracting the virus.
The race gap in deaths is also reflected among age groups. Among people aged between 25 and 54, the prime of their working lives, non-Hispanic Black and Hispanic death rates are much higher than those of whites.
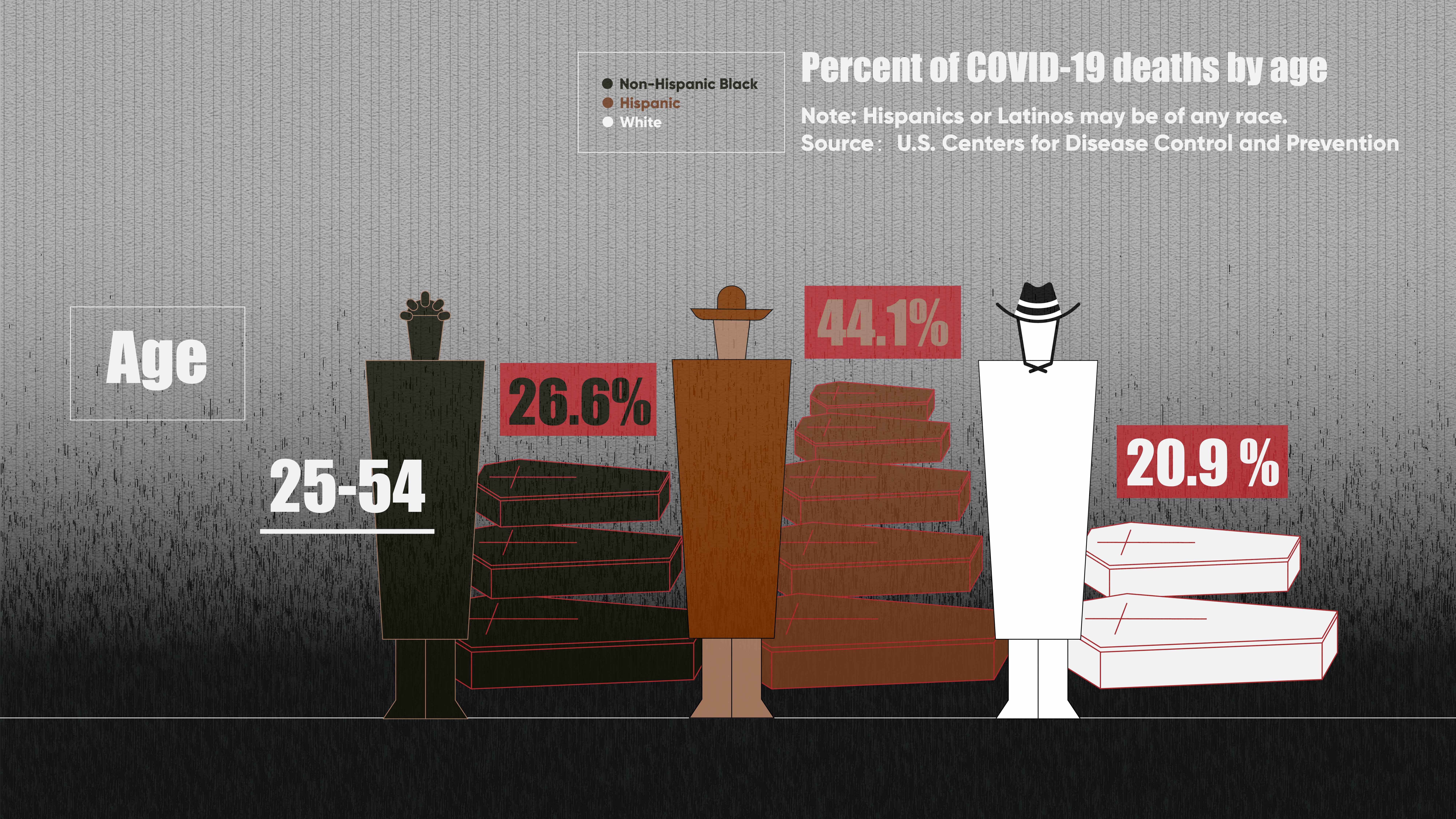
On top of working conditions, pre-existing diseases are a major reason behind racial disparities in COVID-19 complications and deaths. For example, people with diabetes are more likely to have serious symptoms if they are infected with any virus. CDC data indicates that Hispanics and non-Hispanic Black people are more likely to be diagnosed with diabetes, which makes patients more vulnerable to hospitalization and death.
Factors such as inadequate insurance coverage and poor access to healthcare are additional barriers that hinder minorities from affording and receiving appropriate medical treatment in the U.S.
Health inequality is part of racial inequality. This global crisis sheds a brighter light on America's broken healthcare system and long-standing racial disparities. As we know, the virus does not discriminate, but the death toll tells us that people — and the systems they create — do.
(If you want to contribute and have specific expertise, please contact us at opinions@cgtn.com.)

